The following information was adapted from a September, 1997 Fact Sheet entitled Saint Louis Encephalitis: Sometimes A Florida Problem by Dr. Donald Shroyer, currently at the Indian River Mosquito Control District, 5655 41st Street, Vero Beach, FL 32961 (POB 670, Vero Beach, FL 32961-0670), Phone (561) 562-2393, Fax (561) 562-9619. Additional information also may be obtainted from Dr. Charlie Morris, Extension Entomologist, Florida Medical Entomology Laboratory, IFAS-University of Florida, 200 9th Street Southeast, Vero Beach, FL 32962, Phone and Fax (561) 778-7204.
Is the mosquito-transmitted virus disease that is generally considered to be of greatest medical importance in North America. SLE was first recognized in 1933 (in St. Louis, Missouri), and epidemics have occurred sporadically and unpredictably in the subsequent decades. During epidemics large numbers of people may be become seriously ill, and 5% to 30% of those that get the disease die. Major SLE epidemics occurred in Florida in 1959, 1961, 1962, 1977, and 1990. SLE virus also occurs in Central and South America, but rarely causes human disease in those regions.
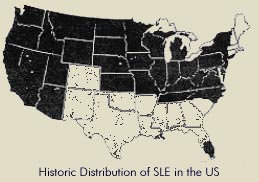 It is important to distinguish between the human disease that we call SLE, and the mosquito-transmitted virus that may cause such disease. Even during epidemics, only a small proportion of individuals actually infected with SLE virus become ill. SLE virus is more common and widely distributed than SLE disease. The virus is a permanent resident of Florida and can be found in some south Florida counties nearly every year.
It is important to distinguish between the human disease that we call SLE, and the mosquito-transmitted virus that may cause such disease. Even during epidemics, only a small proportion of individuals actually infected with SLE virus become ill. SLE virus is more common and widely distributed than SLE disease. The virus is a permanent resident of Florida and can be found in some south Florida counties nearly every year.
However, the causes of epidemics of SLE disease are not known with certainty. Different strains of SLE virus vary substantially in their ability to cause disease. This suggests that epidemics might be caused by the local appearance of a "hot" strain of virus. Risk of epidemics increases when there are exceptionally large numbers of mosquitoes that are capable of transmitting SLE virus. However, periods of epidemic activity in Florida often coincide with periods during which the transmitting mosquitoes are not unusually abundant.
The occurrence and severity of SLE in humans is strongly dependent on age. During epidemics, incidence of disease in people older than 60 is generally 5 to 40 times greater than in those less than 10 years old. Frequency of encephalitis (the most severe symptom associated with SLE) is also age-dependent, increasing from 56% for those age 20 or younger, to 87% for those over 60. Risk of death shows the same trend. Mortality is 7 to 24% among those with SLE and over 50, and less than 5% for those under 50. It is not uncommon for those surviving severe cases of SLE to suffer long term residual neurological damage (known as "sequelae'), which may include paralysis, memory loss, or deterioration of fine motor skills.
It bears repeating that substantial numbers of people are infected with SLE virus, but do not develop recognizable disease. However, those who do become ill face a very serious threat to life. The incubation period from the infective mosquito bite to the first symptoms of SLE is 4 to 21 days, with an average of ten days.
The transmission cycle leading to SLE epidemics is thought to accompany infection of various species of wild birds. A bird infected by the bite of a mosquito can later produce enough virus in its blood to infect other susceptible mosquitoes that might feed upon it. It takes one to two days after infection for the bird to produce significant quantities of virus in its blood, and this virus rapidly disappears one to three days later as the bird recovers from the infection. Thus, there is a narrow "window of opportunity" for the mosquitoes to pick up the virus and then further spread ("amplify") it. After experiencing one SLE infection, an individual bird is forever immune from another SLE infection. SLE virus is not known to cause disease in birds, and birds cannot infect one another.
Under suitable conditions, SLE virus may sufficiently amplify in local bird populations that a large number of mosquitoes are infected, and there is an increased chance that an infected mosquito may bite a human or another incidental viral host. Although SLE virus can produce severe disease in man, humans are poor hosts of the virus; they produce little SLE virus in the blood and are "dead ends" for further virus transmission. As ever greater numbers of susceptible birds recover from SLE infections and become immune, new infections in mosquitoes dwindle unless a substantial number of uninfected migrating birds enter the epidemic zone. Because mosquitoes are short-lived, infected mosquitoes disappear and the epidemic soon ends when the number of susceptable, infected birds is not sustained. As observed during the 1990 Florida SLE epidemic, human infection in South Florida can extend from July through December, which is coincidental with the timing of the annual fall bird migration.

The transmission cycle described above is just one part of the largely unknown, annual life cycle of SLE virus in Florida. We know that the virus is maintained in parts of Florida even in years when we do not detect the virus in birds and mosquitoes. There are mosquito species in Florida that are not suspected of playing a part in the transmission cycle leading to epidemics, yet may nonetheless be important in maintaining the SLE virus life cycle. Of the 72 mosquito species recorded in Florida, only one, Culex nigripalpus, is thought to be important in the amplication and transmission of SLE virus. The role small mammals (e.g. rodents and armadillos) play in maintaining the virus is also unknown.
Unlike birds and man, mosquitoes infected with SLE virus remain infected for life. Fortunately, that life rarely exceeds a week or two. It is surprisingly difficult for an individual mosquito to become infected with SLE virus and transmit that virus by biting another bird or man. Much has to happen before a mosquito can be converted from an uninfected mosquito to a dangerous transmitter of SLE virus.
Not all of the 72 mosquito species that occur in Florida are equally susceptible to infection with SLE virus. Some are incapable of ever transmitting this virus. When a susceptible mosquito takes a blood meal from an infected bird, its stomach cells become infected. After a few days, the virus goes on to infect other organs, including the salivary glands. When salivary glands begin to produce SLE-laced saliva, the mosquito has been transformed into a potential transmitter to any host that it bites.
 Culex nigripalpus shown here is a common Florida mosquito that has been Culex nigripalpuslinked to past SLE epidemics in the state. It is a highly efficient transmitter and its preference to take blood meals from birds favors its involvement in the SLE transmission cycle in Florida. Cx. nigripaipus is a subtropical species and does not occur in most of North America; other Culex mosquitoes serve as the principal SLE transmitters in northern states. Three of these, Cx. quinquefasciatus, Cx. salinarius and Cx. restuans, are common in Florida but have not, as yet, been implicated in SLE transmission in Florida. During past Florida SLE epidemics, several additional mosquitoes were found infected in nature, but it is unknown whether these species are important transmitters. While it is currently believed that Culex nigripalpus is the most important SLE-transmitting mosquito in Florida, it is unwise to ignore the likelihood that other species also contribute to the SLE problem.
Culex nigripalpus shown here is a common Florida mosquito that has been Culex nigripalpuslinked to past SLE epidemics in the state. It is a highly efficient transmitter and its preference to take blood meals from birds favors its involvement in the SLE transmission cycle in Florida. Cx. nigripaipus is a subtropical species and does not occur in most of North America; other Culex mosquitoes serve as the principal SLE transmitters in northern states. Three of these, Cx. quinquefasciatus, Cx. salinarius and Cx. restuans, are common in Florida but have not, as yet, been implicated in SLE transmission in Florida. During past Florida SLE epidemics, several additional mosquitoes were found infected in nature, but it is unknown whether these species are important transmitters. While it is currently believed that Culex nigripalpus is the most important SLE-transmitting mosquito in Florida, it is unwise to ignore the likelihood that other species also contribute to the SLE problem.
During past Florida SLE epidemics, three additional mosquitoes were found infected in nature. Single pools of Aedes taeniorhynchus and an unidentified Culex (Melanoconion) species were found infected with SLE virus. Virus also has been isolated from several pools of Anopheles crucians. The authors feel that it is unlikely that these three species are important transmitters.
SLE virus transmission to birds, and to man during epidemics, is most prevalent from June through November. Populations of Culex nigripalpus also tend to reach their annual peak during this period. While it is impossible to reliably predict epidemic activity, transmission to birds in Florida seems to increase when long periods of drought (10-14 days) are broken by subsequent heavy (greater than two inches) rains. Efforts to monitor SLE virus in Culex nigripaipus in Florida have traditionally focused on the rainy season, but in reality it requires year-round vigilance.
Many mosquito control programs in Florida use "sentinel chickens" to alert them when the threat of SLE is greatest. Chickens are penned in areas where there are mosquitoes. Every two weeks, a blood sample is taken from some of the birds and tested for antibodies to the virus. Chickens seldom become ill when infected with SLE virus. Sentinels were first established throughout Florida in 1978 following a 1977 epidemic of SLE. Though chicken flocks were established to monitor SLE, they also have been used to some extent for EEE, discussed elsewhere.
While sentinels do not forecast SLE or EEE outbreaks, they do provide some limited information on virus activity. Still, the absence of virus activity in chickens does not necessarily mean there is no virus activity. Consequently, sentinel chickens can give a false sense of security regarding EEE or SLE activity. An potential research benefit of sentinel flocks is their abiltiy to confirm via statistical correlation that a developing encephalitis epidemic is probably due to SLE or EEE virus infection. Sentinel chickens have provided us with seasonal and annual patterns of virus activity shown below. Since the mosquito that infected a sentinal chicken is usually long dead before the blood test results are received from the testing laboratory, their use in guiding mosquito control operations is limited. Use of sentinel flocks has been on the decline among mosquito control programs since 1983. Even the Florida Department of Health and Rehabilitative Services, which set up the system, has reduced its support in recent years.
There is no vaccine that can protect against SLE virus infection, and like all virus infections, SLE cannot be cured. Prevention must, therefore, concentrate on minimizing contact between man and transmitting mosquitoes. Individuals can help themselves the most by avoiding being outdoors at night, and especially around sunrise and sunset when mosquitoes seem most active. If they must be out, they should wear long sleeved shirts and long trousers, and apply insect repellent. Mosquito control agencies may help by suppressing mosquito populations with various control methods. Cx. nigripalpus uses a wide variety of semi-permanent or temporary water sources as larval habitats which are often difficult to find or eliminate. Spraying to control adult populations is appropriate in certain circumstances, especially during an epidemic. The explosive nature of epidemics often means that knowledge that an epidemic is underway may come only after peak transmission to man has already passed. This makes it nearly impossible to assess the effectiveness of emergency insecticide applications.
Okaloosa County Mosquito Control District
84 Ready Avenue
Fort Walton Beach, Florida 32548
Phone: (850) 651-7394 or (850) 689-5774
Fax: (850) 651-7397
E-mail
302 N. Wilson St. - Suite 302
Crestview, FL 32536
1250 N. Eglin Parkway, Suite 100
Shalimar, FL 32579
Call 850-689-5050 or 850-423-1542 for all departments.