For more information, check out these links:
University of Florida/Institute of Food & Agricultural Sciences
Horse owners and Veterinarians can sign up for free alerts via the program's website, www.outbreak-alert.com. When a disease report occurs, those who have signed up for the notification and live within a 250-mile radius of the reported outbreak will receive a text or email message to alert them of the potential disease threat.
Owners who travel with their horses and want to stay abreast of disease threats in other parts of the country can enter multiple ZIP codes in the site's search field. They will then be able to receive alerts for all areas they have selected.
The following information was adapted from an August, 1990 article entitled Eastern Equine Encephalitis-A Fatal mistake by Dr. Charlie Morris, Extension Entomologist, Florida Medical Entomology Laboratory, IFAS-University of Florida, 200 9th Street Southeast, Vero Beach, FL 32962, Phone and Fax (561) 778-7204.
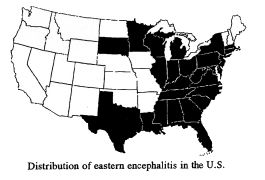
Is also called Eastern Encephalitis (EE), is a fatal disease of humans and horses caused by a virus which is carried by mosquitoes. The disease occurs throughout the eastern United States and Canada from mid-July until first frost in the north, and during most of the year in Florida. Disease outbreaks are usually limited to one to three counties and typically occur every five to ten years. In some locations, however, there may be horse cases every year. The virus that causes the disease is not normally found in either of these animals, thus the disease is truly an accident of nature.
 Any Florida horse from Pensacola to Lake Okeechobee that is located near a freshwater swamp or marsh is at greater risk to EEE. On the average there are 50 to 75 horse cases each year in the State. Over 90% of these animals would die if left alone. Mercifully, once a diagnosis is confirmed, most animals are destroyed. There are typically only one or two human cases each year in Florida. Unfortunately, many are fatal; and of those that do survive, nearly all have some residual effects, particularly mental impairment. There is no specific treatment or cure for EEE in man or horses, but there is a vaccine against the disease in horses.
Any Florida horse from Pensacola to Lake Okeechobee that is located near a freshwater swamp or marsh is at greater risk to EEE. On the average there are 50 to 75 horse cases each year in the State. Over 90% of these animals would die if left alone. Mercifully, once a diagnosis is confirmed, most animals are destroyed. There are typically only one or two human cases each year in Florida. Unfortunately, many are fatal; and of those that do survive, nearly all have some residual effects, particularly mental impairment. There is no specific treatment or cure for EEE in man or horses, but there is a vaccine against the disease in horses.
EEE is caused by a virus called Eastern Equine Encephalomyelitis. The virus is normally found only in wild song birds and in mosquitoes that live in and around wooded swamps; not just any swamp, but a swamp where there is a certain species of mosquito. The EEE mosquito or "black-swamp-mosquito" has the scientific name Culiseta melanura (cuela-see-ta mel-ah-nur-ah). The virus does not usually cause disease in wild birds, although it may cause a temperature, and perhaps a minor illness similar to a cold or flu in a human. It does not affect the mosquitoes in any way.
Culiseta melanura, which translates to "curly black hairs", is indeed a dark mosquito that has a very long proboscis or probe that it uses to draw blood from its hosts. C. melanura has very specific breeding requirements. It occurs in most states east and a few states west of the Mississippi River. The larvae are found only in the underwater root systems of deciduous trees that grow in swamps. Fortunately for us, they get their blood from song birds; rarely do they bite humans or other mammals. And, since C. melanura flies no further than five miles from its breeding sites, most cases of EEE occur within five miles of these swamps.
Well, if C. melanura doesn't bite mammals, how do horses and humans get the disease? The entire story is unknown, but enough facts have been gathered to construct one Florida Model of the life history:
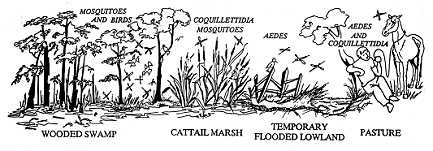
During warm months when C. melanura breeds, there are usually plenty of small birds around for adult mosquitoes to feed on. When female mosquitoes (males do not bite) feed on an infected bird, they pick up the virus. Later, when the mosquito blood feeds on another bird, the virus is transmitted to the new bird. The mosquito remains infected for life and can transmit the virus to all birds it feeds on.
After the mosquito blood feeds, the bird becomes infected and the virus begins reproducing in the bird. In a few days, and for only one or two days, the blood of the bird contains enough virus to infect other mosquitoes that bite it. The bird quickly recovers from the infection and develops immunity. As far as we know, the immunity keeps the birds from becoming infected again. Only newly infected birds can serve as a source of virus for mosquitoes. Therefore, the mosquito seems the most important host as far as virus survival is concerned.
Since C. melanura does not bite people, the key to human and horse infection is tied to the short period when birds have high concentrations of virus in their blood. When other mosquitoes feed on infected birds, they can become infected as well. It is these "secondary" mosquito species that carry the virus to other vertebrate hosts, including horses and humans. For these secondary mosquitoes to transmit the virus from birds to humans, an individual mosquito must successfully blood feed on both groups of animals. Not all mosquito species do that, C. melanura for example.
There is another species of mosquito that is most often associated with outbreaks of EEE in horses and humans. This mosquito, the "salt and pepper mosquito", has the scientific name Coquillettidia perturbans (Coke-qua-la-tid-e ah purr-tur-bans) or "cokes" for short. This is a large black and white mosquito that looks for blood around dusk. Cokes have a geographic distribution similar to C. melanura, but rather than breed in wooded swamps, they breed in cattail or grassy marshes that have a mucky bottom. These types of marshes are often next to the swamps that produce C. melanura.
There may be other mosquitoes, particularly those in the genus Aedes (a-e-dees), that also feed both on birds and mammals and thus could possibly transmit EEE. The species of Aedes involved differ from area to area. Cokes are the only other mosquitoes found throughout the range of EE in the United States. While cokes and Aedes can fly more than five miles, EEE generally does not occur in areas where there are not C. melanura.
Cokes and Aedes can, and do, take blood meals from a variety of other domestic and wild animals; such as cattle, dogs, cats, squirrels, raccoons, and deer. Fortunately, these animals are resistant to the virus and do not develop EEE. Of course, mosquitoes also can blood feed on birds other than wild song birds. Birds that are not native to the U.S., such as ring-necked pheasants and starlings, and some native birds, such as whooping cranes and sandhill cranes can become ill, and many die. Die-off's of exotic birds, particularly pheasants, often precede outbreaks of EEE in humans and horses. Unlike wild birds, infected horses and humans normally do not develop high enough concentrations of virus in their blood to infect mosquitoes. This means that they are not good hosts for the survival of the virus. Once the animal recovers from the infection, or dies, the virus in that animal also dies. Animals like this are called "dead-end hosts", not because they die, but because the virus cannot be perpetuated. Thus, EEE in non-bird hosts is not part of the virus' normal life cycle. It's a fatal mistake for humans, horses and virus alike.
Many mosquito control programs in Florida use "sentinel chickens" to alert them when the threat of EEE is greatest. Chickens are penned in areas where there are mosquitoes. Every two weeks, a blood sample is taken from some of the birds and tested for antibodies to the virus. Chickens seldom become ill when infected with EEE virus. Sentinels were first established throughout Florida in 1978 following a 1977 epidemic of SLE. Though chicken flocks were established to monitor SLE, they also have been used to some extent for EEE, discussed elsewhere.
While sentinels do not forecast SLE or EEE outbreaks, they do provide some limited information on virus activity. Still, the absence of virus activity in chickens does not necessarily mean there is no virus activity. Consequently, sentinel chickens can give a false sense of security regarding EEE or SLE activity. A potential research benefit of sentinel flocks is their abilitabilityy to confirm via statistical correlation that a developing encephalitis epidemic is probably due to SLE or EEE virus infection. Sentinel chickens have provided us with seasonal and annual patterns of virus activity shown below. Since the mosquito that infected a sentinal chicken is usually long dead before the blood test results are received from the testing laboratory, their use in guiding mosquito control operations is limited. Use of sentinel flocks has been on the decline among mosquito control programs since 1983. Even the Florida Department of Health and Rehabilitative Services, which set up the system, has reduced its support in recent years.
The best system to monitor for EEE is to: 1) monitor the population levels of the important mosquitoes, C. melanura, cokes, and man-biting Aedes, 2) test these same species for virus, 3) test native song birds for antibodies to EEE virus, and 4) establish a system to rapidly detect horse cases near the swamps. Since EEE activity in a county during any given year can be limited to a single swamp among many, it is necessary to monitor these factors in all C. melanura breeding swamps.
Florida mosquito control programs typically have a mosquito monitoring system in residential areas. Where there is a potential for EEE, the system should extend to the swamps and marshes. Testing mosquitoes and wild birds for virus activity is more expensive than sentinel chickens, but the test results are more reliable for determining the potential for an EEE outbreak. Unfortunately, today's testing methods are not readily available or cost effective for mosquito control programs. Frequently, horse cases occur before human cases and are used to indicate the spill-over of virus transmission from the bird-mosquito-bird cycle to the bird-mosquito-mammal pathway.
There is a vaccine against EEE for horses; and every horse in the state should be vaccinated and have twice yearly boosters. Unfortunately, there is no vaccine that can protect humans against an EEE virus infection, and like all virus infections, EEE cannot be cured. Prevention must, therefore, concentrate on minimizing contact between man and transmitting mosquitoes.
Individuals can help themselves the most by avoiding being outdoors at night, especially around sunrise and sunset when mosquitoes seem most active. If they must be out, they should wear long sleeved shirts and long trousers, and apply insect repellent. Mosquito control agencies may help by suppressing mosquito populations with various control methods. This means controlling cokes, some Aedes, and particularly, C. melanura. Without C. melanura, there can be no EEE in horses or humans. It is as simple as that.
Larval control is indicated only for prevention, not as a response to an outbreak. Unfortunately, it is usually not practical to spray swamps frequently for C. melanura and coke larva, a practice normally used to control other mosquito species in more residential habitats. Concerted efforts to reduce C. melanura mosquito populations are usually only made after the State Department of Health and Rehabilitative Services declares an EEE alert. Aborting the threat of an EEE outbreak, or an outbreak itself, is most easily done by an aerial application of insecticide to kill adult C. melanura, cokes, and man-biting Aedes. If done properly, only one or two well-timed aerial applications are needed to control the problem for a year. Where aerial application is not possible, less effective ground-based adulticiding techniques may be used to control immigrating carrier mosquitoes.
Okaloosa County Mosquito Control District
84 Ready Avenue
Fort Walton Beach, Florida 32548
Phone: (850) 651-7394 or (850) 689-5774
Fax: (850) 651-7397
E-mail
302 N. Wilson St. - Suite 302
Crestview, FL 32536
1250 N. Eglin Parkway, Suite 100
Shalimar, FL 32579
Call 850-689-5050 or 850-423-1542 for all departments.